My husband Scott was already working with Gabi, a neurofeedback practitioner, for his own reasons. At some point he told her what I was going through with adrenal fatigue. Her response was direct: she thought she could help. That’s how it started. Not with me deciding to try something new. With Scott advocating for me with someone he trusted, and Gabi seeing something worth working on.
Once I understood what neurofeedback actually was, I had my own reasons to show up. I was in the middle of recovering from my second episode of adrenal fatigue, my sleep architecture was still disrupted, and I had read enough about HPA axis dysregulation to understand that the problem wasn’t just about cortisol. My brainwaves had gotten stuck. They had learned to run at high intensity for so long that they had essentially lost the flexibility to do anything else. I needed to retrain that flexibility directly, not just manage the symptoms around it.
What I didn’t expect was what neurofeedback for leaders actually teaches you: what your brain feels like when it finally lets go. That turned out to be the most important thing I learned.
What Is Neurofeedback, Really?
Let’s clear up the most common misconceptions first. Neurofeedback is not electroshock therapy. It is not hypnosis. It is not meditation, though some of what happens during a session might feel meditative. No electricity is sent into your brain. Nothing is done to you without your awareness.
Neurofeedback is biofeedback for your brain. Sensors placed on your scalp read your brainwave activity in real time. That activity feeds into software that rewards your brain for producing target patterns, typically through sound or video that responds to what your brain is actually doing moment to moment. When your brain is producing the target patterns, it gets the reward. When it drifts, the sound shifts to a different tone, a gentle signal nudging it back toward the target state rather than silence or a hard stop. The brain notices, adjusts, and over time learns to find and sustain those more flexible states on its own. The specific setup varies by practitioner and by what your brain needs, and a good practitioner adjusts the protocol as your brain changes.
The formal term is neurofeedback or EEG biofeedback. The underlying principle is operant conditioning applied to brain activity. The brain is remarkably plastic when given the right feedback. It learns. That’s the whole mechanism.
Why Did My Brainwaves Need Retraining?
Here’s what sustained high performance without adequate recovery does over time: it trains your brain to stay on. Not metaphorically. Literally. The neural patterns associated with high activation, problem solving, and vigilance get reinforced through repetition. They become the default. The patterns associated with rest, recovery, and downshifting get used less and less. Eventually the brain loses fluency in them.
This is part of what makes high achiever burnout so different from the kind of burnout most content describes. It doesn’t feel like depletion. It feels like being wired. And even when you want to relax, you can’t. Sleep gets shallower. Recovery gets slower. And because you are still performing, still delivering, still functioning at a level that looks fine from the outside, nothing about your external reality signals that something is wrong. I wrote about why this happens in Why High Achievers Don’t See Burnout Coming — Until Their Body Makes Them Stop.
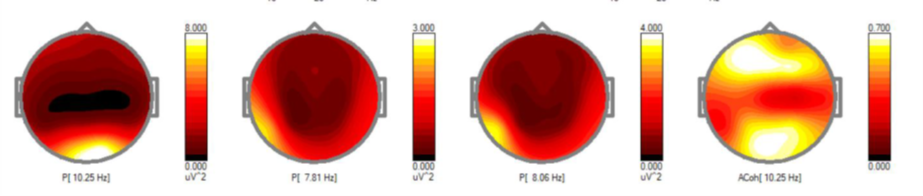
By the time I started neurofeedback, my brain wasn’t stuck in the “on” position anymore. It had already passed that stage. The sustained high-intensity running had finally exhausted itself, and I had crossed into a different kind of stuck: genuine brain exhaustion. I was tired every single minute of every single day. When Gabi did my initial brain scan and looked at the results, she said: your brain is exhausted. I felt immediate relief. Not because it was good news, but because it named exactly what I had been living in and hadn’t been able to explain. That confirmation mattered. The neurofeedback was not the first step in my recovery, but it was the step that made everything else more effective.
What the Sessions Actually Feel Like
I did this almost every week for a year. That is not a casual experiment. That is a commitment, and the results reflect it. You sit comfortably in a chair, sensors attached to your scalp with a conductive gel, nothing invasive. My practitioner, Gabi, would open each session by asking how I was doing. Then she listened. She let me talk through how I was feeling, and she adjusted the protocol based on what she heard. Not a checklist. Not a fixed program I was moving through. She was listening for the whole picture.
In most sessions I chose a video to watch, usually ocean scenes, and tones played in the background as the reward signal. When my brain was producing the target patterns, the tones played. When it drifted, the sound shifted, a gentle different tone that nudged me back toward the target state. Not silence, not a hard stop. More like a soft signal pointing the way. My job was simply to be there. Some sessions I had my eyes closed, just the tones and the instruction to try to stay awake. That last part sounds easy. In the early months it was not. Deep in burnout, the moment the lights dimmed and the office went quiet, my body grabbed the opportunity. I fell asleep. Not because I was bored or inattentive.
Because I was running on a physiological deficit that surfaced the instant the external demands stopped. At home it was the same: lights off, immediately gone. My nervous system had been sprinting for so long that any reduction in stimulation triggered an immediate shutdown.
There were also two sessions I scheduled same day. I had not been my best self that week, both times I had snapped at my boss, and I was not willing to wait for my next appointment to address it. That is just not me. I called Gabi, got in that day, sat down, and told her what happened. She knew exactly what it meant neurologically. It was not a character flaw. It was data. My brainwave patterns were dysregulated enough that the behavior was showing up before I had any conscious awareness of the state I was in. She adjusted the protocol, and we worked on it.
That is what a good practitioner relationship looks like: you can walk in, say what actually happened, and they can do something useful with it. On the first day, before we had done a single session, Gabi handed me a book: Burnout: The Secret to Unlocking the Stress Cycle by Emily and Amelia Nagoski. That told me something about how she understood what I was dealing with. She was not just going to train my brainwaves. She was treating the whole system, and she wanted me to understand the pattern I was living in before we started working on it. That book cracked open a layer I hadn’t yet named. That story belongs in another post.
Across that year of sessions, something shifted. I started to recognize a specific, subtle sensation: a gentle pressure in my forehead, not a headache, not pain, just a kind of quiet density that told me my brain was running hard and hadn’t had a chance to reset. Before neurofeedback, I didn’t know that sensation existed. I would have kept going right through it, the way I always had. Now it was information I could act on.
What Changed in the Data
I got my HUME band after my neurofeedback was complete, which is what makes the data it captures so meaningful. The band was not measuring change in progress. It was measuring what the neurofeedback had built. HRV at 61.8. Deep sleep consistently in the 20 to 25 percent range. REM following. These are not vanity metrics. HRV reflects nervous system flexibility: the capacity to move between activation and recovery states. Deep sleep is when the body does its primary physical repair. REM is when the brain consolidates memory and processes emotion. All three depend on the same underlying thing: a brain that can genuinely downshift.
The neurofeedback retrained that capacity. The HUME band now confirms it is holding. And the 12-minute mindfulness practice I will publish on May 24th is the daily protocol that maintains it, with mid-day HRV tracking showing exactly what happens when I do the practice consistently versus when I skip it.
The data across all three tell a coherent story: neurofeedback as the foundation, the HUME band as the evidence it held, and the daily practice as the maintenance protocol that keeps it running. None of this happened overnight. Neurofeedback is cumulative. The brain changes gradually, not dramatically. But the direction was clear, and the trajectory held.
Why Does This Matter for How You Lead?
Here’s the leadership frame I want to offer, because neurofeedback without a leadership lens is just a health story, and this is not just a health story.
Your brain’s flexibility is a performance asset. Not a wellness concept. Not a nice-to-have. A core component of your capacity to make good decisions, regulate your response under pressure, read the room accurately, and sustain your effectiveness across a full day of demanding work. When that flexibility degrades, you don’t necessarily feel it. You just start operating on a narrower range. You become more reactive. Your prefrontal cortex has less access to the quality of attention it needs. The leadership behaviors you have worked hard to build become harder to execute, not because you have forgotten them, but because the neurological substrate supporting them is running a deficit.
The reactive-to-creative leadership shift that is central to the work we do at EMPOWER2Evolve is not just a mindset shift. It is, at its foundation, a neurological one. You cannot consistently choose a Creator response when your brain is locked in a sustained high-arousal state. You can know exactly what you want to do and still find yourself reacting, because the biology is running a different program. Neurofeedback addresses that layer directly.
Scott understood this before I did. He had watched it play out in high-stakes environments for decades: the leader who knows the right move but cannot access it under pressure. The person whose performance degrades not because of skill gaps but because of a nervous system that never got a chance to reset. His work in the fire service gave him an early window into what brain training could do for people who had spent years operating at the edge of their capacity. That insight was the reason he suggested I try it. It was also, as it turned out, exactly right.
What Comes Next
Neurofeedback was the first step in a recovery protocol that I have built and refined over the past two years. It is what made the next step possible: a daily 12-minute attention training practice grounded in the research of neuroscientist Dr. Amishi Jha. The neurofeedback trained my brain’s flexibility. The daily practice maintains it. I will publish that post on May 24th, and the two posts are meant to be read together.
If you are a high-performing leader who is still functioning, still delivering, and starting to notice that recovery is taking longer than it used to, I want to be direct with you: that is data. Your body is already telling you something. The question is whether you are building in the conditions to hear it, and whether you have tools that work at the level where the problem actually lives.
The Bottom Line
Neurofeedback for leaders is not a fringe concept or a wellness trend. It is direct training for the neurological flexibility that underlies every leadership behavior you are trying to build and sustain. When high performance has trained your brain to stay on, and the cumulative cost of that is showing up in your sleep, your recovery, and the narrowing range of your responses under pressure, the intervention needs to work at the level of the brain itself. That is what neurofeedback does. It does not fix you. It gives your brain the feedback it needs to find its own way back to flexible, and that changes everything downstream.
In Your Lab This Week
Reflection: Think about the last time you genuinely felt your brain slow down. Not tired. Not distracted. Actually slow, quiet, and rested. How long ago was that? What does the gap between that memory and your current baseline tell you?
Practice: If neurofeedback is something you want to explore, start by finding a qualified practitioner. The ISNR directory at isnr.org is a good place to start. You do not need a referral or a diagnosis. You need a practitioner who can read your baseline and set training goals that fit your situation. If you are not ready to go that far yet, the 12-minute flashlight practice I will publish on May 24th is the daily maintenance practice that works alongside neurofeedback, or on its own, to build attentional flexibility. Watch for it.
This post is part of a series on the physiological foundations of high performance. If you haven’t read the anchor post yet, start at High Achiever Burnout Signs for the full context on why high achievers miss the signals their body is sending.
Frequently Asked Questions
What is neurofeedback and is it safe?
Neurofeedback is a form of biofeedback that trains brainwave activity using real-time feedback. Sensors read your brain’s electrical patterns; a software program rewards adaptive patterns by keeping a video or audio signal running smoothly. No electricity is sent into the brain. It is non-invasive and has been in clinical and research use for decades. The International Society for Neuroregulation and Research maintains a practitioner directory and research library at isnr.org for those who want to review the evidence base.
How is neurofeedback different from meditation?
Meditation asks you to direct your attention using your own will and practice. Neurofeedback gives your brain direct feedback on its own activity and lets it learn through that feedback loop, without requiring you to consciously guide the process. The two can be complementary. In my experience, neurofeedback created the neurological flexibility that made my daily mindfulness practice more accessible and more effective. But they are different tools working through different mechanisms.
How many sessions does it take?
This varies by individual and by what is being trained. Most practitioners discuss results in terms of a course of sessions rather than a single visit, typically somewhere in the range of 20 to 40 sessions for meaningful change, though some people notice shifts earlier. I worked with a practitioner over an extended period as part of a broader recovery protocol. If you are considering neurofeedback, work with a qualified practitioner who can assess your specific brainwave patterns and set appropriate training goals.
Is neurofeedback only for people with a medical diagnosis?
No. While neurofeedback has clinical applications for specific conditions, it is also used by high performers who are not in crisis but want to optimize their brain’s flexibility, focus, and recovery capacity. My own use was in that category: not a mental health crisis, but a brain that had gotten stuck in patterns that were no longer serving my performance or my health. The question worth asking is not whether you have a diagnosis, but whether your brain’s current patterns are giving you what you need.
References
International Society for Neuroregulation and Research (ISNR). Practitioner directory and research library. isnr.org
Frontiers in Psychology (2025). Chronic Stress in Relation to Clinical Burnout: An Integrative Scoping Review.
Ring, M. (2025). Integrative medicine approaches to HPA axis recovery. American Journal of Medicine.
Wentz, I. (2023). Adrenal Transformation Protocol. HarperCollins.
Nagoski, E. and Nagoski, A. (2019). Burnout: The Secret to Unlocking the Stress Cycle. Ballantine Books.
